Kneecap
The kneecap, also called the patella, is a flat, disc-shaped bone sheathed with articular cartilage on the back to create a sliding surface.
When this cartilage surface wears out, damage can occur that can lead to early onset osteoarthritis in the long term.
The most common cause of retropatellar cartilage damage is when the kneecap is improperly guided across its shallow groove (also called patellar instability or patellar subluxation), due, for example, to a muscular deficit or an injury such as patellar dislocation. This causes the kneecap to increase pressure on the trochlea, damaging the cartilage layer.
Depending on the cause and type of patellar dislocation, treatment can be either surgical or conservative.
More questions?
Our experts are happy to help you
Just give us a call!

LATERALISATION OF THE PATELLA/PATELLAR SUBLUXATION:
A deviation of the patella from the articular surface may occur congenitally, through a lack of muscular direction, or as a result of previous patellar injuries. This is called lateralisation of the patella or patellar subluxation. The deviation from the articular surface leads to increased contact pressure of the patella on the articular surface, which can result in damage to the joint cartilage and thus arthrosis. There is often not only pain but also a pronounced joint noise behind the kneecap.
The treatment of choice is a relieving incision, which can be carried out using arthroscopy, to reduce the exterior pull on the patella and to optimize the pulling direction with concomitant capsulorrhaphy on the medial side. This evenly redistributes the pressure behind the kneecap, giving the damaged cartilage the potential to heal. Otherwise, additional treatment measures (see cartilage) are required. Physiotherapy can and should be commenced shortly after the operation.
KNEECAP DISLOCATION (PATELLAR-DISLOCATION):
Dislocation of the patella (kneecap dislocation) from the femoral groove can occur at any age. It is a problem more common for young girls and women and more rarely occurs in young boys and men. Depending on the anatomy, patellar dislocation occurs due to a pre-existing weakness in the muscles and ligaments or from the application of force. In all cases, the medial groove of the patella ruptures and causes the patella to dislocate, i.e. spring out to the side. The patella often does not stay in that lateral position but instead springs back spontaneously. This repositioning can cause injuries in the area of the cartilage. An X-ray will show significant tilting and lateral displacement of the patella in images of the kneecap as well as smaller cracked splinters. Treatment approach depends on the position of the patella following dislocation and the diagnosis of cartilage damage.
In many cases, there is a predisposition for patellar dislocation (habitual dislocation), which is more common for women than men. This caused by a malformation of the patellar guide channel (trochlear hypoplasia), depriving the patella of a guide trough and providing instead only an inclined plane. As a result of this predisposition, the patella fails to develop correctly, and a so-called Jägerhut patella occurs (see also Wiberg classification of patella shapes).
TREATMENT:
When knee joint effusion is pronounced - which is often the case - arthroscopic surgery is recommended, as blood and blood byproducts can damage the cartilage. Before the arthroscopic procedure, blood is removed from the joint, and the cartilage surfaces are examined for any damage. Larger avulsion fractures can be reattached using arthroscopy or open surgery. In most cases, however, the primary problem is a fracture in the area of the medial patellofemoral ligament (MPFL). Depending on the age of the patient, the injury, and the misalignment, Dr. Gäbler recommends one of the following types of treatment.
- In the case of a very slight malposition, which can be diagnosed using X-ray or arthroscopy, consistent physiotherapy is carried out, regardless of age or gender. Physiotherapy helps center the patella and strengthen the musculature that pulls the kneecap medially. A clinical check and X-ray imaging are carried out again after three months of therapy to help decide if treatment can be concluded.
- If there is an older injury, the patient is elderly, or if the malposition has already balanced itself out well with a flexed position of 20°, arthroscopic relief of weight-bearing on the lateral fixation apparatus (lateral release) is completely adequate. It must be confirmed, however, using MRI, that the medial patellofemoral ligament (MPFL) is intact! Optimal guidance of the patella can be achieved during physiotherapeutic follow-up care (the same as stated above). A clinical follow-up check and X-ray imaging are also carried out here after three months.
- If it is a fresh dislocation, the patella is clearly at an angle, and interior tearing is extensive, arthroscopic or open suturing and shortening of the MPFL is recommended. A lateral release is indicated only in exceptional cases, as it has been shown that lateral release surgery can lead to patellar instability. After the operation, the knee is immobilized with a splint for four weeks. Patients should not put weight on the knee for the first 14 days and must use crutches to walk. The return to bearing weight progresses according to the degree of pain. It is possible to begin physiotherapy as early as two weeks after the operation. After six weeks, physical therapy should be accompanied by strength training, and patients should have a clinical check-up and X-ray after three months.
- If patellar dislocation has already occurred several times (recurrent patellar dislocation), a precise clinical examination must be carried out: if there is hypoplasia of the articular surface, the patella is stable in a flexed position of 90°, something has to be carried out on the articular surface; is the medial femoropatellar ligament (MPFL) that stabilizes the patella in a medial direction intact? What does the cartilage behind the patella look like?
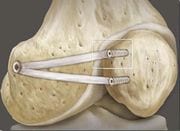
After the operation, the knee is immobilized with a splint for six weeks. In the first two weeks, no weight bearing is permitted and the knee joint should not be flexed by more than 30°. The patient can then bear half of their body weight after two weeks and the leg can be flexed up to 90° (for another four weeks). The splint can be removed after six weeks if progress is normal. Physiotherapy is commenced immediately.
PATELLAR DISLOCATION IN CHILDREN AND ADOLESCENTS:
Die öfters auftretende Kniescheibenluxation kann schon im Kindes- oder Jugendlichenalter zu schweren Knorpelzerstörungen an der Rückseite der Kniescheibe führen, mit freien Knorpelstücken im Gelenk und der Gefahr der frühzeitigen Arthrose. Nach Abklärung der Beinachse und des Gleitlagers, sollte man NICHT auf den Wachstumsabschluss warten, sondern so rasch als möglich eine MPFL Rekonstruktion durchführen – so wie man ja auch bei instabiler Kreuzbandsituation bei Kindern und Jugendlichen das vordere Cruciate Ligament ersetzen sollte, um frühzeitige Gelenkzerstörungen zu verhindern.
click here for literature references
More questions?
Our experts are happy to help you
Just give us a call!




